Between a congressional effort to finish daylight savings time, a Latest York Times feature on timed drug delivery, and reviews of circadian biology in several major journals, circadian medicine has had a buzzy yr. The joy is especially high amongst oncology researchers.
At various intervals for the reason that Seventies, long before the molecular gears of the circadian clock were understood, timed delivery of cancer medication has gave the impression to be just over the horizon. In 1979, when a bunch of oncologists published the paper “On methods for testing and achieving cancer chronotherapy,” cancer was the second most typical reason for death in America, following heart disease. In 2020, the same was true — but cancer was catching up. Within the intervening 40 years, scientists have learned an enormous amount about how cancer works and how one can treat it. Some cancers that after would have been a death sentence are actually curable. Others have remained intractable despite many years of study and billions of dollars of research investment.
Now, with a greater understanding of the molecular underpinnings of humans’ circadian clocks and more sophisticated measurements of physiological phenomena, researchers are taking a fresh run at the thought of circadian cancer therapy.
“There may be an immense excitement (in the sector),” said Francis Lévi, a French oncologist who has worked for many years on basic mechanisms and clinical studies of chronochemotherapy. He and his colleagues say they’ve begun to look at that drugs might be simpler, or cause fewer negative effects, if delivered at certain times of day.
But others point to the long and disappointing history of circadian medicine as a reason to be cautious in regards to the hype. The clock, said biochemist Aziz Sancar, “interfaces with the whole lot. It’s logical to think that it should have an impact … but you’ve got to show it experimentally.”
If treating cancer higher were so simple as using the identical drug at a distinct time of day, Sancar argues, wouldn’t we all know that by now?
Day by day rhythms of disease
Anyone who has awoken at 4 a.m. after a long-distance trip knows that the circadian cycle is a robust regulator of human behavior. Its rhythms can also regulate disease. Individuals with rheumatoid arthritis feel essentially the most pain within the morning, while gout and asthma attacks are greater than twice as likely at night. Individuals with Alzheimer’s disease are likely to develop into upset and uneasy around sundown.
Responses to external stimuli change by time of day too. In a famous experiment from the Sixties, mice injected at noon with lipopolysaccharide, a bacterial toxin mimicking sepsis, died 80% of the time; those injected at midnight died just 20% of the time. Conversely, some cholesterol drugs are best taken at night, when cholesterol synthesis is highest.

An illustration by biophysicist Irina Bezsonova shows a portion of the CLOCK
protein’s three-d structure.
Clock disruption and carcinogenesis
Does circadian disruption cause cancer? In humans, the reply has gave the impression to be yes. But preclinical models have yielded confusing results. Read more
Disruption of circadian rhythms has been linked to diseases, especially cancer. In epidemiological studies of shift staff, disruption to clock functions has been linked sometimes, but not at all times, with higher cancer rates (see “Clock disruption and carcinogenesis”). Meanwhile, studies on a wide range of cancer biopsies indicate that some retain a each day cycle in clock proteins and proliferate in each day waves, but their timing relative to the remaining of the body can vary.
In a recent study of breast cancer metastasis within the journal Nature, researchers at several hospitals in Switzerland reported that blood samples taken at 4 a.m., when patients normally could be asleep, contained many more circulating tumor cells than samples taken at 10 a.m. Cells from every time point also showed different growth profiles. When grafted into mice, the nighttime cells grew way more aggressively, suggesting that, independent of number, they is perhaps higher capable of seed metastases.
Using transcriptomics, the researchers showed that circulating tumor cells captured at night expressed many genes related to mitosis, while those collected by day devoted more energy to translation and ribosome biogenesis. Oddly, nonetheless, the tumor cells also appeared to don’t have any cellular time keeper; that they had lost oscillation of their clock proteins.
How the cellular clock runs
The molecules that run the human circadian clock are expressed in almost every cell. The primary described was a protein called CLOCK, short for “circadian locomotor output cycles kaput.” CLOCK works with binding partner BMAL1 as a transcription factor. When the 2 bind unfettered to DNA, they drive transcription of diverse genes. But that free access is feasible for less than a part of the day. More often than not, BMAL and CLOCK have additional binding partners that disrupt their ability to bind to DNA.
Their window of opportunity peaks slightly after midday. As evening nears, their transcriptional activity produces a bunch of inhibitor proteins called cryptochromes, or CRYs, and period proteins, or PERs. When a cryptochrome binds the CLOCK–BMAL dimer, it recruits a pile-on of other proteins that becomes a robust repressive complex.
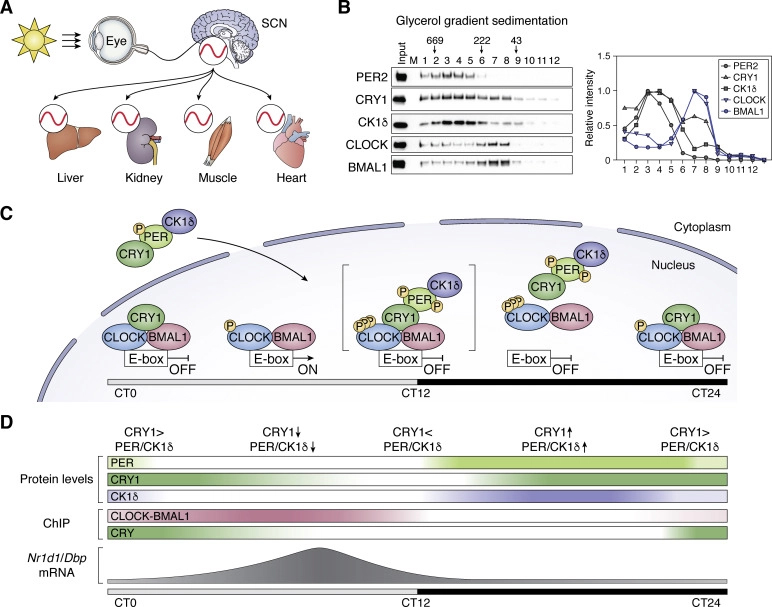
YANG ET AL., J BIOL CHEM 2021
A figure from a recent review within the Journal of Biological Chemistry shows how complexes form and separate, regulating DNA expression to generate circadian rhythms.
One kinase within the complex regularly phosphorylates CLOCK. Carrie Partch, a structural biologist on the University of California, Santa Cruz, who works on the assembly and variety of circadian protein complexes, said that the enzyme’s inefficiency is a feature, not a bug. “We expect that clocks depend on poor enzymes to assist add the delay that results in a 24-hour (cycle).”
By nightfall, CLOCK and BMAL are incapacitated. They chill out their hold on the DNA. This turns off the tap of CRY and PER protein production. Because the night wears on, degradation reduces levels of CRYs and PERs, while phosphatases reverse CLOCK phosphorylation. As that happens, CLOCK and BMAL regain their ability to bind to DNA. One CRY, with especially high binding affinity, sticks around until dawn — at which point, it too begins to be degraded, eventually freeing CLOCK–BMAL to transcribe again.
Boiled all the way down to its barest essentials, the cycle is easy. Night: off. Day: on. Repeat at roughly 24-hour intervals in almost every cell within the body. The central clock within the brain corrects any slippage.
The central clock
That central clock consists of a cluster of neurons near the optic nerve, called the suprachiasmatic nucleus, or SCN, which receives light information directly from the retina, independent of the visual system.
Erik Herzog, a professor at Washington University in St. Louis, studies SCN function and communication. “In the identical way we predict in regards to the atomic clock in Boulder, Colorado, sending out a pulse every morning at 3 a.m. … the SCN sends out each day signals to get everybody on local time,” Herzog said.
If a smartwatch were cut off from the atomic clock, it will proceed to run but might drift out of accuracy. The identical is true for cells: Each can oscillate by itself, but signals from the SCN keep them synchronized. Other parts of the brain turn pulses from the SCN into fluctuations in body temperature and circulating hormones melatonin and cortisol, each of which peaks at a signature time of day.
The SCN is a robust pacesetter, but its control, researchers recently have learned, shouldn’t be absolute. A brief list of tissues, particularly within the skin and cornea, respond on to light, even when the SCN has been rigged to run on a distinct schedule than an animal’s external environment. Also, in the midst of human aging, central and peripheral clocks lose synchronicity.
Still, the SCN has a crucial coordinating role. For instance, it is vital to determining an individual’s chronotype, or each day behavior pattern. Not every individual responds to light cues the identical way; polymorphisms in clock genes, including the CRY and PER genes that mediate the CLOCK–BMAL pile-on, can determine how long a person’s clock takes to finish a cycle — probably because they alter the kinetics of protein complex formation, Partch said. Manipulating those genes in just the SCN might be enough to alter an animal’s chronotype and switch a morning mouse to a night mouse.
Whatever its inherent speed, because the cycle repeats itself in cells, it produces an ambient rhythm in gene expression. Nearly half of coding genes, and lots of noncoding RNAs, show circadian patterns in no less than one tissue. Those transcripts affect the proteome, metabolome and cellular behaviors equivalent to the cell cycle, DNA damage responses and apoptosis. Physiological functions equivalent to sleep, body temperature, immune activity and feeding vary by time of day. Small wonder that researchers are asking whether medical interventions may additionally answer to the clock.
In discussions of medication and the circadian rhythm, two kinds of interventions come up. A physician or a patient might try to regulate the clock through light therapy, timing cues equivalent to exercise, or small molecules that interfere with the circadian oscillatory system. Or they could attempt to time medicines to succeed in their highest efficacy by working with biochemical and behavioral patterns that oscillate each day.
Drugging the clock
Scientists have found some evidence that bringing patients’ circadian rhythms into alignment using light and other cues might be useful. Timing food intake and exercise may help with Type 2 diabetes, and some (but not all) studies have concluded that cycling light conditions in a neonatal intensive care unit speeds development. But small molecules that alter the function of individual clock proteins have, to date, had little effect.
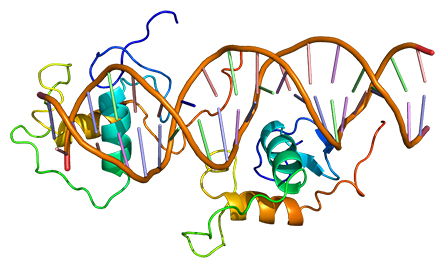
ZHAO ET AL. MOLECULAR CELL 1998
REV-ERB is a transcription factor, shown here binding to DNA.
The clock is difficult to drug, in accordance with pharmacologist Tom Burris of the University of Florida, whose lab developed agonists for the clock protein called REV-ERB, a nuclear receptor that regulates BMAL1 expression. The drugs’ effects on mice are subtle; to see them, his lab needed to dose the animals after that they had been at the hours of darkness for several days. He thinks that’s because clock proteins are highly redundant, making the circadian cycle robust.
“I don’t think we will reset your entire rhythm, but we will modulate pieces of it,” Burris said. Because various clock proteins link to assorted other cell systems, he added, tweaking a few of them is perhaps useful, even when REV-ERB activation doesn’t reset the sleep–wake cycle altogether.
Several groups have studied the results of the REV-ERB agonists on tumor cells. Sometimes, their effects look promising. A lab on the Salk institute observed that they appeared to reduce autophagy and cause programmed cell death selectively in cancer cells. Nevertheless, critics indicate that the drugs even have effects in mice that lack the REV-ERB gene, suggesting that they might act through other targets.
Burris expects that, over time, “we’re going to grasp more about how the oncogenic pathways are coupled to the circadian rhythm and have the opportunity to hijack a few of the targets which might be shared.”
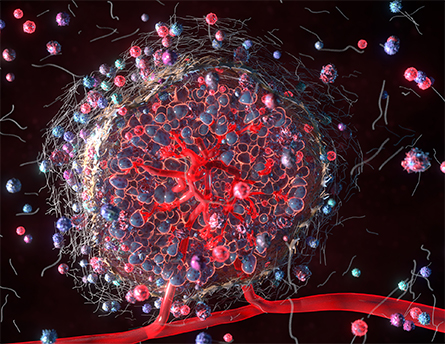
The number and metastatic potential of circulating cancer cells can change by time
of day. Researchers hope to search out the optimal time to make use of drugs that concentrate on proliferation.
Still, for this reason complexity, more physicians have focused on timing a drug for biggest efficacy. Jeffrey Field, a pharmacologist on the University of Pennsylvania, put it this fashion: “The evidence for drugging the clock might be weaker than clocking the drugs.”
Clocking the drugs
An influential review article published within the journal Science in 2019 found that 75% of 106 trials testing the identical drug at two times of day showed differences in either toxicity or efficacy. Roughly 20 of those trials tested cancer drugs. Drugs with a shorter half-life were more prone to show a time-of-day effect.
In a study that cited that work, researchers within the labs of Jeffrey Field and Penn colleague Amita Sehgal tested 126 drugs at six-hour intervals, comparing their effects on osteosarcoma cells that had a functioning circadian clock and others that didn’t. They found that the timekeeping cells were more sensitive to about half of the drugs at some times of day than at others. Specializing in a bunch of medication that concentrate on the chaperone protein HSP90, which they previously had shown connects the clock with the cell cycle, they found that they were only if given just after the chaperone hit its lowest each day expression level.
“Proliferation was affected because a particular a part of the cell cycle was regulated by the clock, and that a part of the cell cycle can also be targeted by many chemotherapeutics,” Sehgal, a circadian biologist, said.
On this case, timing the drug to match the circadian clock meant also timing it to match the cell cycle, which the clock can influence. Sehgal and Field proposed that links between the cell cycle and circadian rhythm could also be amongst an important reasons that some drugs show circadian effects. But other pathways also fluctuate with time of day: Researchers have suggested exploiting rhythms in DNA repair or inflammation, each of which interact with the clock, to get essentially the most out of extant drugs. Unraveling causality in these complex interactions could be a challenge.
“Often I get the query, ‘Is the efficacy that you just’re getting since you’re regulating the circadian system or another piece?’” Burris said. “I’ve often said, you simply can’t say that, because they’re connected.”
Besides hitting a goal at the suitable time — which can mean that concentrate on concentration is high or low, depending on the drug — there’s a second mechanism by which dosing time might give a drug a bonus: It could cause lower toxicity at certain times of day. Most legacy chemotherapy drugs kill healthy and tumor cells somewhat indiscriminately, causing harmful negative effects. Whether it’s killing more cancer cells or damaging other tissues less, improvement to a drug’s therapeutic index — the space between an efficient dose and a dose that causes harmful negative effects — could possibly be useful.
Finally, a drug could also be metabolized in a different way over time. Besides the specified goal and any collateral proteins that cause off-target effects, molecules which will cycle include the liver enzymes that convert a drug to its lively form, the transporters that carry it into its goal cell or across the blood–brain barrier, the enzymes required for degrading or secreting it, and other players that deliver an lively pharmaceutical ingredient to the tissue where it acts.
Sehgal suggested that retrospective studies of people that occur to take a drug at different times are an excellent strategy to scan for effects without getting lost in mechanistic details. “Perhaps that’s not the optimal time from the attitude of the each day rhythm in cortisol, but perhaps it’s from the viewpoint of when the goal is up.”
Confusing clinical trials
Russell Van Gelder, a physician–scientist who chairs the ophthalmology department on the University of Washington, is skeptical that dosing at a particular time of day will yield dramatic medical advances. He said, “You’re taking extremely complicated physiologies which have multiple clock components running at the identical time and assuming that there’s some phase that’s optimized and can have a really clear effect.”
He cited a history of clinical failures to indicate conclusive circadian effects. For instance, a 2006 study of timed chemotherapy for patients with metastatic colorectal cancer found that timed dosing only helped some patients. Median survival was comparable between the study’s arms, but timed therapy reduced the chance of an earlier death in men by 25% and increased it by 38% in women.
Nobody is definite why women fared worse than men on this study. Creator Francis Lévi, the oncologist in France, vehemently disputed the characterization of this study as a failure. Lévi’s group subsequently has conducted many studies defining the lowest-toxicity timing for various chemotherapies and continues to look at sexual dimorphism in optimal dosage times. He said, “It’s a fancy issue, and that is why it has taken a protracted time and shouldn’t be yet finished.”
But when a recent news article on circadian medicine cited the study but only mentioned the improved survival amongst men, Aziz Sancar, a biochemist on the University of North Carolina who shared the 2015 Nobel Prize for discovery of a DNA repair enzyme that helps to set the clock, was galvanized to talk up about his doubts in regards to the field at large. Sancar’s lab had hung out searching for evidence that an optimal time exists when DNA-damaging chemotherapeutic agents is perhaps only.
Doubled survival time amongst men, Sancar said, simply wasn’t what the 2006 study reported. “That got distorted, and hastily people said chronotherapy cures cancer.”
Many clinical trials of timed chemotherapy have varied not only the time when drug is run, but additionally the infusion regimen or length or the entire dosage, making their results difficult to interpret.
Meanwhile, Sancar remained concerned in regards to the half of study participants who had fared worse on timed treatment. “He felt that … this enthusiasm for timed chemotherapy could actually be harming people, or subgroups of individuals, and never helping them,” said longtime colleague Van Gelder.
In two review articles published back to back last yr in the journal Science (with co-author Van Gelder) and the Journal of Biological Chemistry (with colleagues from UNC), Sancar laid out an argument that enthusiasm for chronochemotherapy exceeded the evidence that supports it.
Sancar’s argument is very detailed but returns to several themes: He says that the chronochemotherapy literature glosses over negative data, overstates positive findings in reviews and generalizes inappropriately from small studies.
For instance, he pointed to a widely cited 1985 paper reporting that a bunch of 31 women with ovarian cancer who received adriamycin within the morning and cisplatin within the evening experienced fewer negative effects than those whose treatment schedule began within the evening; that study couldn’t be replicated, Sancar said. In a study of hundreds of patients with metastatic ovarian and uterine cancers, he added, the Gynecology Oncology Research Group “concluded that chronotherapy didn’t help.”
In an interview, Sancar also bemoaned widespread bias against publishing negative results, especially in the event that they contradict previous findings. He said that he desires to see rigorous tests of the chronochemotherapy hypothesis considered objectively — including the disappointing studies.
Summing up their joint work, Van Gelder said, “It’s not that circadian rhythms don’t have anything to do with cancer. They’ve a terrific deal to do with cancer. It’s very clear that tumors disrupt rhythmicity, rhythmicity governs tumors, and there are deep mechanistic relationships between clock genes and oncogenes. Nevertheless, the relationships don’t readily predict the suitable timing for treatment.”
Presented with these critiques, Lévi wrote, “An ophthalmologist and a biochemist can hardly understand the methodologic constraints of clinical research and the way much we learn from them to advance medicine regardless of hypothesis validation.” One vital finding from clinical studies, he said, has been that there is critical divergence between individual responses based on sex, lifestyle and genotype, meaning that drug timing probably will should be personalized to be effective.
Lévi also cited a recent systematic review of chronochemotherapy studies that appeared within the Lancet Oncology. The review considered 18 clinical trials published from 1994 to 2021; Lévi was an creator of six of them. Most investigated the results of dosage timing on infused chemotherapeutic drugs, especially mixtures including cisplatin and oxaliplatin. The study found that 11 of the 18 trials reported a discount in toxicity, or harmful negative effects, and none showed any reduction in efficacy. Nevertheless, the review’s authors cautioned, it was unattainable to isolate the results of timing, since most of the studies also had altered the duration of infusions or the general dosage patients received.
The case of temozolomide
“Historically, the research hasn’t been done fastidiously,” admitted Erik Herzog, the Washington University biologist. That makes it difficult for researchers to get support to check recent circadian medicine hypotheses, equivalent to the one he has been working on with WUSTL colleagues Joshua Rubin, a neuroscientist, and Jian Campian, a neurooncologist.
Herzog and Rubin teamed up to review timing in glioblastoma. They became enthusiastic about temozolomide, or TMZ, one of the best available treatment. The drug works by alkylating purine bases in DNA, causing double-strand breaks that halt replication. Patients take the pill each day for five days, take three weeks off to recuperate, and repeat indefinitely. TMZ has been a front-line treatment since 2005, however it’s no panacea; a glioblastoma patient can expect to continue to exist average 16 months after diagnosis.
Emily Slat, a student in Herzog’s lab, found that cultured glioblastoma cells from each mice and humans keep a each day rhythm, and the time after they receive TMZ matters. Treating tumor cells early within the day killed many more of them. Herzog said that the timed effect seems to depend upon DNA repair, not cell proliferation.

ATIKA ATIKAWA / WIKIMEDIA COMMONS
Despite the challenges, many researchers expect chronochemotherapy to be proven
effective eventually. An inventive rendering shows the CLOCK protein.
“In case you give temozolomide at a time of day when the clock is revved up and driving the expression of repair enzymes, chances are you’ll not have much success with the drug,” Herzog said. “Actually, there are occasions of day when it looks like temozolomide does almost nothing.”
When she saw the outcomes, Campian was intrigued but cautious. “I didn’t wish to pull off a big study, put in lots of resources, after which it doesn’t work,” she said.
Many treatments, she knew, have looked promising in preclinical models, only to fail in patients. Besides, trials are expensive. A principal investigator must pay institutional review board fees, compensate research assistants to screen and enroll patients and keep records so as, and devote staff time to analyzing data. Regardless that the drug in query already was prescribed to almost every patient on the clinic, it was difficult to secure pharmaceutical firms’ interest without patent protection. When Campian wrote grants to the National Cancer Institute and a number of other foundations, those groups also didn’t bite.
As an alternative, the team found an experiment already underway at their clinic. Many physicians, Campian said, recommend that patients take TMZ within the evening, when the nausea and fatigue it causes could also be easier to bear. Other doctors recommend that or not it’s taken within the morning.
WUSTL had a various enough group of prescribers for a retrospective study, which was easier to rearrange since it will not impact clinical decisions. Amongst 166 patients who had passed through the clinic and whose dosing time could possibly be determined, the study team found no difference in survival time between groups. Nevertheless, amongst patients with methylation of the gene for DNA repair enzyme MGMT — a biomarker that physicians already know sensitizes cells to TMZ treatment — they saw a dramatic profit from morning dosing.
Campian and Herzog next planned a small feasibility study that the university supported. They’d ask patients to take TMZ either within the morning or the evening and compare their outcomes. Contrary to received wisdom, they found that amongst thirty-five patients on different dosing schedules, no significant differences in hostile negative effects arose. Nevertheless, there was also no significant difference in survival.
“It dissatisfied us, of course,” Herzog said. But, he added, the study was too small to detect a positive effect reliably, especially one which may apply only to patients with methylated MGMT. As well as, the team didn’t control for patients’ chronotypes, or for disruptions to circadian rhythm that the cancer itself could cause. Continuing the study, the team has begun to make use of wearable activity monitors to find out how a patient’s internal clock compares to the wall clock.
To find out of course whether there may be any difference between taking TMZ within the morning and the evening, doctors would want to recruit several hundred patients, Campian said. She’d wish to run such a study, because to her it seems more promising to get the best possible efficacy out of a drug that already has been shown to be effective and secure — secure, no less than, as chemotherapeutic agents go — than to run the risks of developing a recent treatment. She said that she is dissatisfied that funders don’t appear to agree.
“It’s going to be a protracted time before (chronochemotherapy) becomes the norm, primarily due to expense,” Herzog said. He added that studies that start through the use of cultured cells from patients to discover the times of greater drug efficacy for a person could also be a cheaper way forward.
Herzog said that almost all physicians and grant reviewers expect timing to have at best a light effect on how well medicine works. He predicts that if robust evidence on one drug could possibly be collected, it will help make the case for circadian therapies. But without much industry interest, it isn’t clear how such a blockbuster finding could occur.
“Once a drug company would show something, the others will too,” Lévi said. But he thinks that the industry as a complete is conservative and that no company is prone to move first on an idea that has failed prior to now.
From chemotherapy to immunotherapy
At a recent American Society for Clinical Oncology meeting, Lévi counted five abstracts showing circadian effects of assorted drugs in several cancers. “I believe the thrill about timing, and the magnitude of the profit, is now a crucial fact,” he said.
Lots of those drugs were antibodies, a few of which activate the immune system. In contrast with broad-spectrum DNA-disrupting agents, these are biological drugs with single specific targets and will lend themselves to cleaner mechanistic hypotheses, Van Gelder said. Although they’ve very long half-lives, which blunts the results of dose timing in small molecules, some antibodies have shown significant time-of-day effects, a puzzle nobody has explained yet.
Immunotherapies, which recruit quiescent immune cells, may profit from the immune system’s strong inherent circadian rhythms. Checkpoint inhibitors, antibodies that block a mechanism cancer cells use to evade immunity, are an example; one evaluation suggests they may go best when more T cells can infiltrate the tumor and worst when T cell infiltration is low.
Some practical questions on implementing chronochemotherapy are closer than ever to being answered. For instance, if a drug works best at certain times of day, do clinicians must determine whether a patient has a certain chronotype, or whether their individual tumor is cycling, before moving forward with treatment? Clinical researchers can control for patient chronotypes during trials using wearable activity monitors. To find out whether a tumor is in phase with its host, researchers may culture a tumor biopsy and add a luciferase reporter of circadian gene expression; or they might isolate circulating tumor cells and use an algorithm to guage the transcriptome and determine its point within the circadian cycle.
“We’d like to find out who’re the patients with good rhythms, who’re the patients with poor rhythms, and determine whether chronotherapy will likely be kind of effective,” Lévi said. But so long as it stays difficult to finance studies of chronochemotherapy, he added, “We is not going to know. We is not going to advance.”
Despite the challenges of demonstrating a conclusive effect for chronochemotherapy, many researchers expect the approach to bear fruit eventually, especially because the tools for personalized medicine improve doctors’ ability to tailor treatment plans for people.
Still, Van Gelder said, “I believe the chances that we’re going to search out some drug that is totally ineffective at one circadian phase and phenomenally effective at one other are fairly low.” In any case, most drug targets that fluctuate in response to the clock change by at most just a few fold. “They don’t go from zero to a thousand.”
Nonetheless, Sancar said, the prospect of curing cancer with circadian rhythms is an appealing one, even for him. “All scientists, all human beings want their work to be relevant.”
Clock disruption and carcinogenesis
Does circadian disruption cause cancer? In humans, the reply has gave the impression to be yes. But preclinical models have yielded confusing results, making it hard to say why individuals who do shift work develop cancer at higher rates in epidemiological studies.
“It’s been almost a two-decade-long conversation now,” said biologist Carrie Partch on the University of California, Santa Cruz. “I don’t think there’s a very clear answer … when it comes to ‘a specific cancer has a specific style of effect on the clock,’” or a specific disruption of the clock promoting particular cancers.
In mouse models, she said, removing different clock genes from different genetic backgrounds has led to results which might be difficult to match. In cell lines, it may possibly be tricky to decide on an appropriate control for an oscillating tumor tissue.
In response to Aziz Sancar on the University of North Carolina at Chapel Hill, publication bias — the tendency for positive results to get more attention than negative findings — makes it harder to guage the evidence. For instance, he described a colleague who had difficulty publishing her remark that, contrary to a previous high-profile paper, mice lacking two Period genes don’t show higher cancer rates than their unmodified relatives.
In response to French oncologist Francis Lévi, there are no less than eight kinds of cancer whose prognosis is significantly worse if circadian signaling is disrupted. But studies even have shown that cancer — and its associated stress and difficult medical treatments — can disrupt sleep, which can impair circadian rhythms. The complex causal relationships complicate not only studies of whether circadian disruption could cause cancer but additionally studies concerning chronochemotherapy.





